What is Glaucoma?
Glaucoma is a group of diseases that damage the eye’s optic nerve and
can result in vision loss and blindness. However, with early detection
and treatment, you can often protect your eyes against serious
vision loss.
The optic nerve
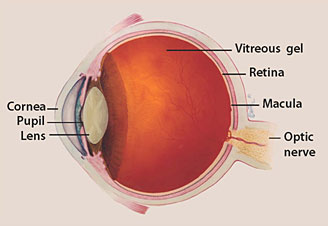
The
optic nerve is a bundle of more than 1 million nerve fibers. It
connects the retina to the brain. (See diagram above.) The retina is the
light-sensitive tissue at the back of the eye. A healthy optic nerve is
necessary for good vision.
How does the optic nerve get damaged by open-angle glaucoma?
Several large studies have shown that eye pressure is a major risk
factor for optic nerve damage. In the front of the eye is a space called
the anterior chamber. A clear fluid flows continuously in and out of
the chamber and nourishes nearby tissues. The fluid leaves the chamber
at the open angle where the cornea and iris meet. (See diagram below.)
When the fluid reaches the angle, it flows through a spongy meshwork,
like a drain, and leaves the eye.
In open-angle glaucoma, even though the drainage angle is “open”, the
fluid passes too slowly through the meshwork drain. Since the fluid
builds up, the pressure inside the eye rises to a level that may damage
the optic nerve. When the optic nerve is damaged from increased
pressure, open-angle glaucoma-and vision loss—may result. That’s why
controlling pressure inside the eye is important.
Another risk factor for optic nerve damage relates to blood pressure.
Thus, it is important to also make sure that your blood pressure is at a
proper level for your body by working with your medical doctor.
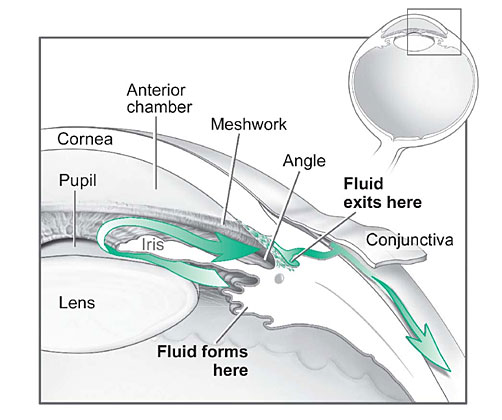
Fluid pathway is shown in teal.
Can I develop glaucoma if I have increased eye pressure?
Not necessarily. Not every person with increased eye pressure will
develop glaucoma. Some people can tolerate higher levels of eye pressure
better than others. Also, a certain level of eye pressure may be high
for one person but normal for another.
Whether you develop glaucoma depends on the level of pressure your
optic nerve can tolerate without being damaged. This level is different
for each person. That’s why a comprehensive dilated eye exam is very
important. It can help your eye care professional determine what level
of eye pressure is normal for you.
Can I develop glaucoma without an increase in my eye pressure?
Yes. Glaucoma can develop without increased eye pressure. This form
of glaucoma is called low-tension or normal-tension glaucoma. It is a
type of open-angle glaucoma.
Who is at risk for open-angle glaucoma?
Anyone can develop glaucoma. Some people, listed below, are at higher risk than others:
- African Americans over age 40
- Everyone over age 60, especially Mexican Americans
- People with a family history of glaucoma
A comprehensive dilated eye exam can reveal more risk factors,
such as high eye pressure, thinness of the cornea, and abnormal optic
nerve anatomy. In some people with certain combinations of these
high-risk factors, medicines in the form of eyedrops reduce the risk of
developing glaucoma by about half.
Glaucoma Symptoms
At first, open-angle glaucoma has no symptoms. It causes no pain. Vision stays normal. Glaucoma can develop in one or both eyes.
Without treatment, people with glaucoma will slowly lose their
peripheral (side) vision. As glaucoma remains untreated, people may miss
objects to the side and out of the corner of their eye. They seem to be
looking through a tunnel. Over time, straight-ahead (central) vision
may decrease until no vision remains.

Normal Vision.

The same scene as viewed by a person with glaucoma.
How is glaucoma detected?
Glaucoma is detected through a comprehensive dilated eye exam that includes the following:
Visual acuity test. This eye chart test measures how well you see at various distances.
Visual field test. This test measures your
peripheral (side vision). It helps your eye care professional tell if
you have lost peripheral vision, a sign of glaucoma.
Dilated eye exam. In this exam, drops are placed in
your eyes to widen, or dilate, the pupils. Your eye care professional
uses a special magnifying lens to examine your retina and optic nerve
for signs of damage and other eye problems. After the exam, your
close-up vision may remain blurred for several hours.
Tonometry is the measurement of pressure inside the
eye by using an instrument called a tonometer. Numbing drops may be
applied to your eye for this test. A tonometer measures pressure inside
the eye to detect glaucoma.
Pachymetry is the measurement of the thickness of
your cornea. Your eye care professional applies a numbing drop to your
eye and uses an ultrasonic wave instrument to measure the thickness of
your cornea.
Can glaucoma be cured?
No. There is no cure for glaucoma. Vision lost from the disease cannot be restored.
Glaucoma Treatments
Immediate treatment for early-stage, open-angle glaucoma can delay
progression of the disease. That’s why early diagnosis is
very important.
Glaucoma treatments include medicines, laser trabeculoplasty,
conventional surgery, or a combination of any of these. While these
treatments may save remaining vision, they do not improve sight already
lost from glaucoma.
Medicines. Medicines, in the form of eyedrops or
pills, are the most common early treatment for glaucoma. Taken
regularly, these eyedrops lower eye pressure. Some medicines cause the
eye to make less fluid. Others lower pressure by helping fluid drain
from the eye.
Before you begin glaucoma treatment, tell your eye care professional
about other medicines and supplements that you are taking. Sometimes the
drops can interfere with the way other medicines work.
Glaucoma medicines need to be taken regularly as directed by your eye
care professional. Most people have no problems. However, some
medicines can cause headaches or other side effects. For example, drops
may cause stinging, burning, and redness in the eyes.
Many medicines are available to treat glaucoma. If you have problems
with one medicine, tell your eye care professional. Treatment with a
different dose or a new medicine may be possible.
Because glaucoma often has no symptoms, people may be tempted to stop
taking, or may forget to take, their medicine. You need to use the
drops or pills as long as they help control your eye pressure. Regular
use is very important.
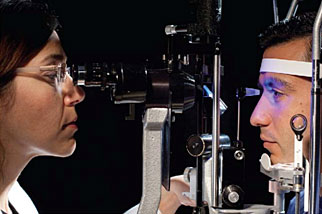
A tonometer measures pressure inside the eye to detect glaucoma.
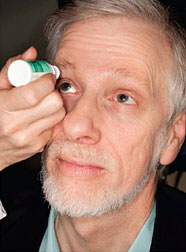
Make sure your eye care professional shows you how to put the drops
into your eye. For tips on using your glaucoma eyedrops, see the inside
back cover of this booklet.
Laser trabeculoplasty. Laser trabeculoplasty helps
fluid drain out of the eye. Your doctor may suggest this step at any
time. In many cases, you will need to keep taking glaucoma medicines
after this procedure.
Laser trabeculoplasty is performed in your doctor’s office or eye
clinic. Before the surgery, numbing drops are applied to your eye. As
you sit facing the laser machine, your doctor holds a special lens to
your eye. A high-intensity beam of light is aimed through the lens and
reflected onto the meshwork inside your eye. You may see flashes of
bright green or red light. The laser makes several evenly spaced burns
that stretch the drainage holes in the meshwork. This allows the fluid
to drain better.
Like any surgery, laser surgery can cause side effects, such as
inflammation. Your doctor may give you some drops to take home for any
soreness or inflammation inside the eye. You will need to make several
follow-up visits to have your eye pressure and eye monitored.
If you have glaucoma in both eyes, usually only one eye will be
treated at a time. Laser treatments for each eye will be scheduled
several days to several weeks apart.
Studies show that laser surgery can be very good at reducing the
pressure in some patients. However, its effects can wear off over time.
Your doctor may suggest further treatment.
Conventional surgery. Conventional surgery makes a
new opening for the fluid to leave the eye. (See diagram on the next
page.) Your doctor may suggest this treatment at any time. Conventional
surgery often is done after medicines and laser surgery have failed to
control pressure.
Conventional surgery, called trabeculectomy, is performed in an
operating room. Before the surgery, you are given medicine to help you
relax. Your doctor makes small injections around the eye to numb it. A
small piece of tissue is removed to create a new channel for the fluid
to drain from the eye. This fluid will drain between the eye tissue
layers and create a blister-like “filtration bleb.”
For several weeks after the surgery, you must put drops in the eye to
fight infection and inflammation. These drops will be different from
those you may have been using before surgery.
Conventional surgery is performed on one eye at a time. Usually the operations are four to six weeks apart.
Conventional surgery is about 60 to 80 percent effective at lowering
eye pressure. If the new drainage opening narrows, a second operation
may be needed. Conventional surgery works best if you have not had
previous eye surgery, such as a cataract operation.
Sometimes after conventional surgery, your vision may not be as good
as it was before conventional surgery. Conventional surgery can cause
side effects, including cataract, problems with the cornea,
inflammation, infection inside the eye, or low eye pressure problems. If
you have any of these problems, tell your doctor so a treatment plan
can be developed.
What are some other forms of glaucoma and how are they treated?
Open-angle glaucoma is the most common form. Some people have other types of the disease.
In
low-tension or
normal-tension glaucoma,
optic nerve damage and narrowed side vision occur in people with normal
eye pressure. Lowering eye pressure at least 30 percent through
medicines slows the disease in some people. Glaucoma may worsen in
others despite low pressures.
A comprehensive medical history is important to identify other
potential risk factors, such as low blood pressure, that contribute to
low-tension glaucoma. If no risk factors are identified, the treatment
options for low-tension glaucoma are the same as for
open-angle glaucoma.
In
angle-closure glaucoma, the fluid at the front of
the eye cannot drain through the angle and leave the eye. The angle
gets blocked by part of the iris. People with this type of glaucoma may
have a sudden increase in eye pressure. Symptoms include severe pain and
nausea, as well as redness of the eye and blurred vision. If you have
these symptoms, you need to seek treatment immediately.
This is a medical emergency.
If your doctor is unavailable, go to the nearest hospital or clinic.
Without treatment to restore the flow of fluid, the eye can become
blind. Usually, prompt laser surgery and medicines can clear the
blockage, lower eye pressure, and protect vision.
In
congenital glaucoma, children are born with a
defect in the angle of the eye that slows the normal drainage of fluid.
These children usually have obvious symptoms, such as cloudy eyes,
sensitivity to light, and excessive tearing. Conventional surgery
typically is the suggested treatment, because medicines are not
effective and can cause more serious side effects in infants and be
difficult to administer. Surgery is safe and effective. If surgery is
done promptly, these children usually have an excellent chance of having
good vision.

Conventional surgery makes a new opening for the fluid to leave the eye.
Secondary glaucomas can develop as complications of other medical conditions. For example, a severe form of glaucoma is called
neovascular glaucoma,
and can be a result from poorly controlled diabetes or high blood
pressure. Other types of glaucoma sometimes occur with cataract, certain
eye tumors, or when the eye is inflamed or irritated by a condition
called uveitis. Sometimes glaucoma develops after other eye surgeries or
serious eye injuries. Steroid drugs used to treat eye inflammations and
other diseases can trigger glaucoma in some people. There are two eye
conditions known to cause secondary forms of glaucoma.
Pigmentary glaucoma occurs when pigment from the iris sheds off and blocks the meshwork, slowing fluid drainage.
Pseudoexfoliation glaucoma occurs when extra
material is produced and shed off internal eye structures and blocks the
meshwork, again slowing fluid drainage.
Depending on the cause of these secondary glaucomas, treatment
includes medicines, laser surgery, or conventional or other
glaucoma surgery.
What research is being done?
Through studies in the laboratory and with patients, NEI is seeking
better ways to detect, treat, and prevent vision loss in people with
glaucoma. For example, researchers have discovered genes that could help
explain how glaucoma damages the eye.
NEI also is supporting studies to learn more about who is likely to
get glaucoma, when to treat people who have increased eye pressure, and
which treatment to use first.
What You Can Do
If you are being treated for glaucoma, be sure to take your glaucoma
medicine every day. See your eye care professional regularly.
You also can help protect the vision of family members and friends
who may be at high risk for glaucoma-African Americans over age 40;
everyone over age 60, especially Mexican Americans; and people with a
family history of the disease. Encourage them to have a comprehensive
dilated eye exam at least once every two years. Remember that lowering
eye pressure in the early stages of glaucoma slows progression of the
disease and helps save vision.
Medicare covers an annual comprehensive dilated eye exam for some
people at high risk for glaucoma. These people include those with
diabetes, those with a family history of glaucoma, and African Americans
age 50 and older.
What should I ask my eye care professional?
You can protect yourself against vision loss by working in
partnership with your eye care professional. Ask questions and get the
information you need to take care of yourself and your family.
What are some questions to ask?
About my eye disease or disorder…
- What is my diagnosis?
- What caused my condition?
- Can my condition be treated?
- How will this condition affect my vision now and in the future?
- Should I watch for any particular symptoms and notify you if they occur?
- Should I make any lifestyle changes?
About my treatment…
- What is the treatment for my condition?
- When will the treatment start and how long will it last?
- What are the benefits of this treatment and how successful is it?
- What are the risks and side effects associated with this treatment?
- Are there foods, medicines, or activities I should avoid while I’m on this treatment?
- If my treatment includes taking medicine, what should I do if I miss a dose?
- Are other treatments available?
About my tests…
- What kinds of tests will I have?
- What can I expect to find out from these tests?
- When will I know the results?
- Do I have to do anything special to prepare for any of the tests?
- Do these tests have any side effects or risks?
- Will I need more tests later?
Other suggestions
- If you don’t understand your eye care professional’s responses, ask questions until you do understand.
- Take notes or get a friend or family member to take notes for you.
Or, bring a tape recorder to help you remember the discussion.
- Ask your eye care professional to write down his or her instructions to you.
- Ask your eye care professional for printed material about your condition.
- If you still have trouble understanding your eye care professional’s answers, ask where you can go for more information.
- Other members of your healthcare team, such as nurses and pharmacists, can be good sources of information. Talk to them, too.
Today, patients take an active role in their health care. Be an active patient about your eye care.
Loss of Vision
If you have lost some sight from glaucoma, ask your eye care
professional about low vision services and devices that may help you
make the most of your remaining vision. Ask for a referral to a
specialist in low vision. Many community organizations and agencies
offer information about low vision counseling, training, and other
special services for people with visual impairments.
How should I use my glaucoma eyedrops?
If eyedrops have been prescribed for treating your glaucoma, you need
to use them properly, as instructed by your eye care professional.
Proper use of your glaucoma medication can improve the medicine’s
effectiveness and reduce your risk of side effects.
To properly apply your eyedrops, follow these steps:
- Wash your hands.
- Hold the bottle upside down.
- Tilt your head back.
- Hold the bottle in one hand and place it as close as possible to the eye.
- With the other hand, pull down your lower eyelid. This forms a pocket.
- Place the prescribed number of drops into the lower eyelid pocket.
If you are using more than one eyedrop, be sure to wait at least 5
minutes before applying the second eyedrop.
- Close your eye OR press the lower lid lightly with your finger for
at least 1 minute. Either of these steps keeps the drops in the eye and
helps prevent the drops from draining into the tear duct, which can
increase your risk of side effects.

















